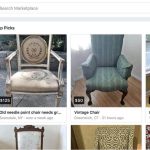
How To View Messages On Facebook Marketplace

How To View Messages On Facebook Marketplace: Facebook Marketplace has grown to be one of Meta’s most successful projects since ...
Read more
How To View Your Items Listings On Facebook Marketplace

How To View Your Items Listings On Facebook Marketplace: Facebook has been a popular social media platform for quite a ...
Read more
How to Add Marketplace to Your Facebook Account
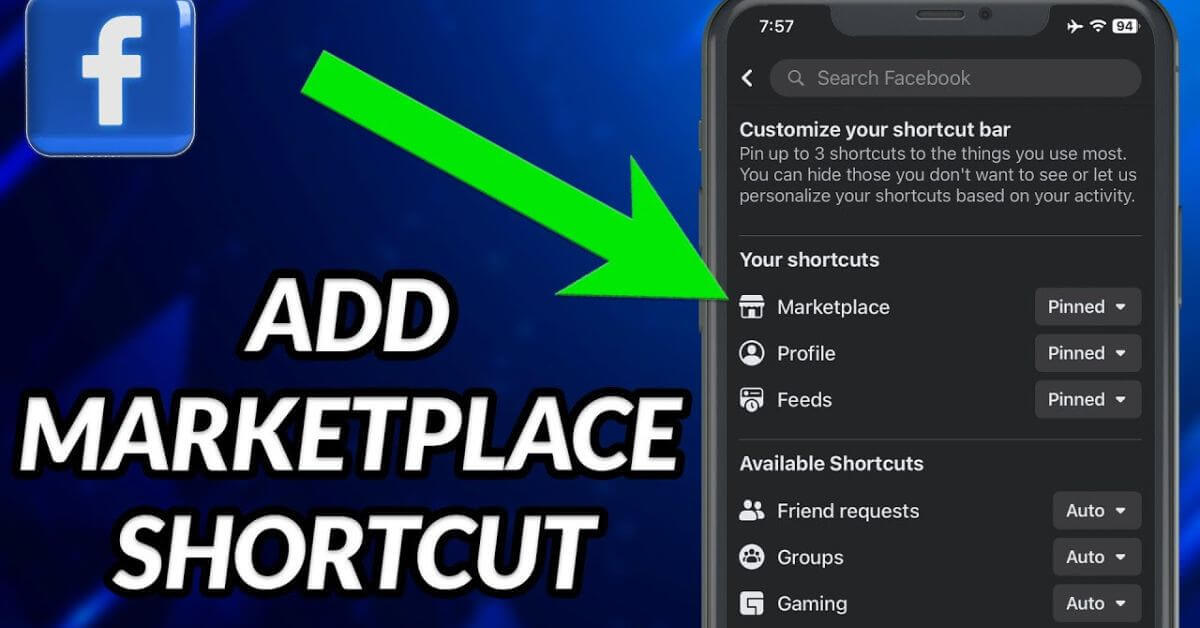
How to Add Marketplace to Your Facebook Account: Have you ever sought the rush of clearing out your home and ...
Read more
How To Find Who Follows You On Facebook

How To Find Who Follows You On Facebook: Facebook profiles may be quite private spaces. You might not want just ...
Read more
How To Recover Deleted Messages On Facebook Messenger

How To Recover Deleted Messages: There’s a good possibility that you have inadvertently erased communications between you and your friends ...
Read more
Finding and Buying Durable Furniture on Facebook Marketplace
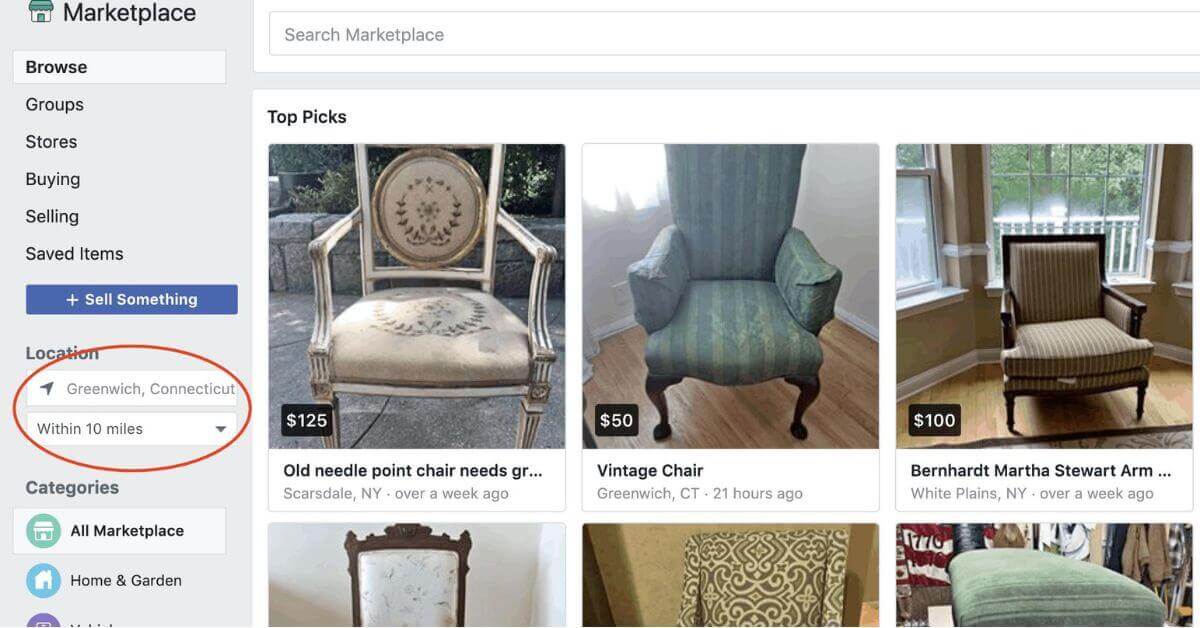
Finding and Buying Durable Furniture: In recent times, the Facebook marketplace has become a one-stop shop for various items ranging ...
Read more
Facebook Marketplace Cars for Sale – Used 2021 Chevrolet Spark Near Me

Facebook Marketplace Cars for Sale: Some models are distinguished in the realm of automotive excellence due to their unique blend ...
Read more
How to See Who Viewed your Facebook profile

How to See Who Viewed your Facebook profile: Ever questioned who might be viewing your Facebook profile? Over the years, ...
Read more
How to Get Facebook Marketplace Icon on Mobile Devices

How to Get Facebook Marketplace Icon on Mobile Devices: If you are using the Facebook app, “Marketplace” is one of ...
Read more
How to Locate Facebook Marketplace Free in 2024 | On Desktop, Android, and iOS

How to Locate Facebook Marketplace Free: Facebook Marketplace is a free feature that is accessible to all Facebook users. The ...
Read more